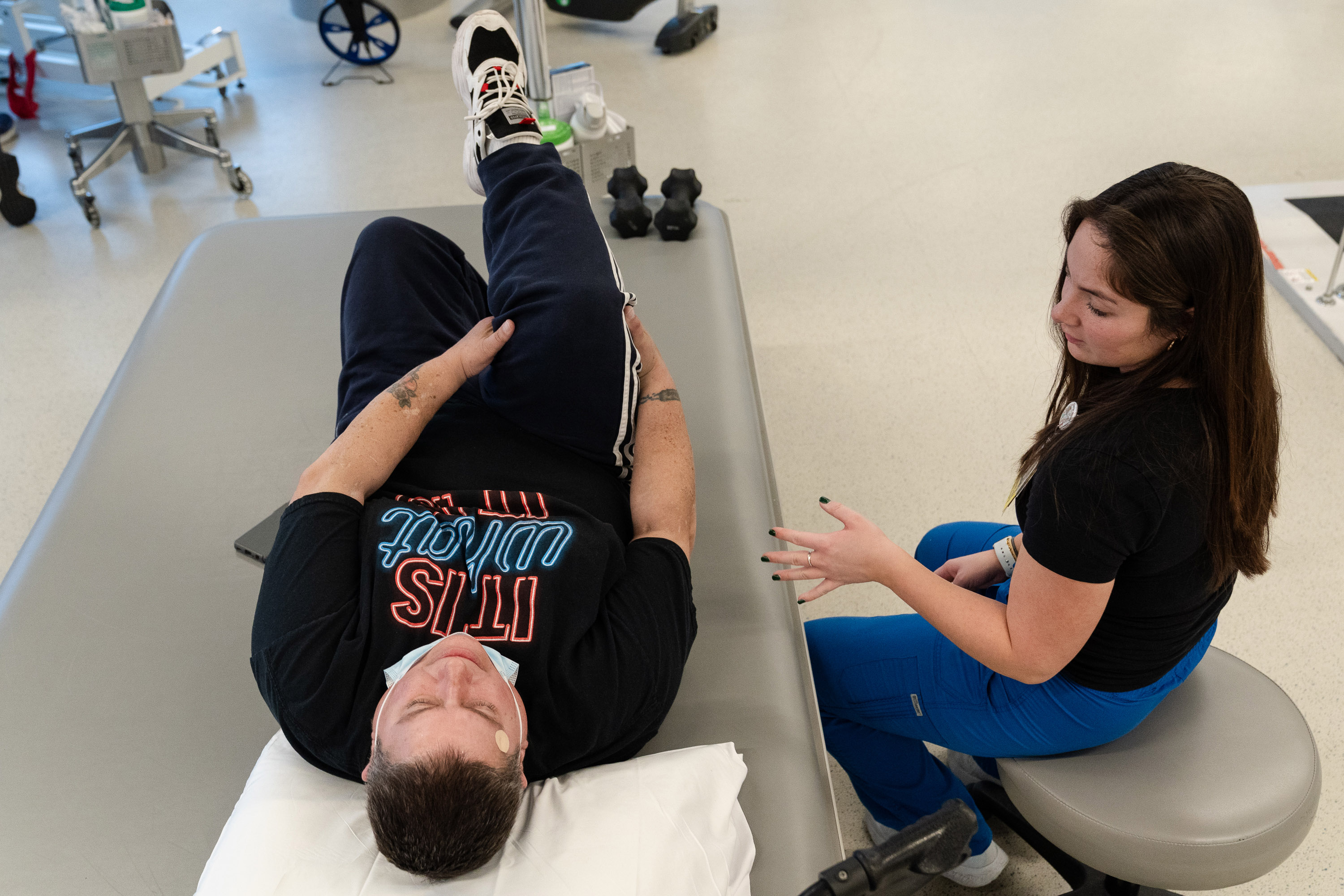
A Fortina Hernández la llaman “la que lo sabe todo”.
Durante más de dos décadas, esta trabajadora de salud comunitaria ha ayudado a cientos de familias del sureste de Los Ángeles a inscribirse en programas de ayuda alimentaria, ha informado sobre seguros médicos asequibles y ha ayudado con medicamentos para sus afecciones crónicas. Su frase favorita: “más vale prevenir que curar”.
Pero sólo gana unos $20 la hora en una organización de salud comunitaria y tiene un segundo trabajo para poder llegar a fin de mes. “Nos pagan muy poco y esperan demasiado”, dijo. “Generamos confianza. Ofrecemos apoyo. Somos el hombro en el que muchos se apoyan, pero no recibimos un salario justo”.
California buscaba profesionalizar a miles de trabajadores de salud comunitarios como Hernández. La meta era mejorar la salud de las poblaciones inmigrantes, en particular los residentes hispanos, que a menudo padecen mayores tasas de enfermedades crónicas, son más propensos a no tener seguro médico y se enfrentan a más barreras culturales y lingüísticas para acceder a servicios.
Estudios demuestran que su trabajo puede reducir las hospitalizaciones, y las visitas a las salas de emergencias y a las clínicas de urgencias.
El estado siguió al pie de la letra una serie de recomendaciones de expertos publicadas en 2019 para estandarizar la formación y la certificación de estos profesionales. Así, poder integrarlos a las plantillas de trabajadores de salud y ofrecerles salarios justos, incluyendo reembolsos a través de Medi-Cal, el Medicaid estatal, para compensar el trabajo que tradicionalmente se ha realizado de forma voluntaria o con salarios bajos.

Pero seis años después, California ha dado marcha atrás en muchas de esas iniciativas.
El estado ha eliminado un programa de certificación y ha recortado casi toda la financiación para formar y ampliar esta plantilla, a pesar de que se había fijado el objetivo de contar con 25.000 trabajadores para este año.
Aunque Medi-Cal comenzó a cubrir sus servicios, los planes de salud participantes establecieron requisitos de facturación desiguales, lo que dificulta que los trabajadores obtengan el reembolso. Además, el estado no cumplió con el aumento salarial previsto.
Con los recortes de fondos federales recién aprobados y el foco del presidente Donald Trump en la deportación de inmigrantes, incluso compartiendo datos personales de Medicaid con el Departamento de Seguridad Nacional, los activistas temen que California abandone su iniciativa de equidad en la salud para los inmigrantes, las personas de color y las personas con bajos ingresos. En un momento en el que, aseguran, esa labor es más necesaria que nunca.
“Estamos en una situación muy grave en este momento”, afirmó Cary Sanders, directora en la California Pan-Ethnic Health Network, una organización estatal que aboga por la equidad en la salud.
Elana Ross, vocera del gobernador Gavin Newsom, dijo que “el estado ha tomado medidas difíciles pero necesarias para garantizar la estabilidad fiscal” y que la administración sigue dialogando con los trabajadores de salud comunitarios.
Ross agregó que el gobernador demócrata, posible candidato a la presidencia, sigue comprometido con la defensa de los inmigrantes perseguidos por la administración Trump.

“Nuestra oficina está en la calle”
Hay más de 60.000 trabajadores de salud comunitarios en todo el país, incluidos unos 9.200 en California, y se prevé que esta fuerza laboral crezca un 13% en la próxima década, tres veces más rápido que el conjunto de todas las profesiones, según datos de 2024 de la Oficina de Estadísticas Laborales de Estados Unidos.
Sin embargo, expertos afirman que estas cifras están subvaloradas, dada la variedad de títulos que poseen estos trabajadores y el hecho de que muchos no trabajan en el cuidado de salud propiamente dicho ni en instituciones gubernamentales.
“Trabajador de salud comunitario” es un término genérico que incluye a distintos tipos de trabajadores. A menudo conocidos como promotores, suelen ser mujeres que trabajan en clínicas, hospitales, departamentos de salud pública y organizaciones sin fines de lucro locales, en lugares en los que se les tiene confianza y donde conocen las necesidades más urgentes de su comunidad.
Además de ayudar a las personas a controlar afecciones crónicas como las cardiopatías y la diabetes, promueven la salud reproductiva, la salud infantil y la higiene bucal, y ayudan a las personas mayores con demencia a prevenir lesiones y manejar sus medicamentos.
Pueden hacer que las personas se sientan seguras al denunciar la violencia doméstica y otros abusos. También las conectan con servicios de asistencia para la vivienda y la alimentación. “El trabajador de salud comunitario no se sienta en un escritorio”, dijo Hernández. “Nuestra oficina está en la calle”.
En 2019, la California Future Health Workforce Commission recomendó integrar a estos trabajadores en el sistema de salud, y en 2022, el estado autorizó $281 millones durante tres años para el Departamento de Acceso e Información de Salud de California, que supervisa el desarrollo del personal de este sector, con el fin de reclutar, formar y certificar a estos trabajadores.
La agencia trató de estandarizar la formación y la certificación, pero algunos grupos comunitarios temían que eso creara barreras de acceso al no dar suficiente crédito a la experiencia y a la competencia cultural.
Pero el año pasado, justo cuando la agencia ofrecía más flexibilidad y permitía la formación basada en el trabajo comunitario, el estado recortó $250 millones en financiación debido a restricciones presupuestarias. Este año, el programa de certificación ha sido oficialmente eliminado.
El vocero Andrew DiLuccia señaló que la agencia establecerá un programa para acreditar a las organizaciones comunitarias en lugar de a los trabajadores individuales y que tiene previsto gastar los $12 millones restantes en asistencia técnica, desarrollo de la fuerza laboral y salarios para quienes trabajan con las comunidades inmigrantes.
Según la National Academy for State Health Policy, otros 32 estados ofrecen algún tipo de programa de certificación para trabajadores de salud comunitarios ya sea voluntario o bien obligatorio.
Algunos activistas afirman que California está perdiendo la oportunidad de establecer una trayectoria profesional para esta mano de obra. Muchos de los cursos que ofrecen hoy en día por organizaciones sin fines de lucro, condados y universidades requieren el pago de una cuota, un título, dominio del inglés o experiencia previa. La mayoría se concentran en el área de San Francisco o Los Ángeles, lo que crea desiertos de formación en gran parte del estado.

Lourdes Bernis, una dentista de Ecuador, es un ejemplo de cómo los trabajadores de salud comunitarios podrían integrarse en el sistema de salud. Comenzó como promotora voluntaria hace más de una década y en 2019 recibió formación gratuita del condado de Los Ángeles, lo que le permitió conseguir un trabajo a tiempo completo, con beneficios, en el Departamento de Salud Mental del condado para ayudar a mujeres hispanohablantes a gestionar la depresión y la ansiedad mientras se recuperan del consumo de drogas.
Bernis ahora quiere convertirse en especialista de apoyo entre pares en hospitales y clínicas. Mientras tanto, muchos de sus colegas con décadas de experiencia siguen atrapados en puestos mal pagados y no pueden permitirse costear cursos de formación para avanzar. “Hay promotoras que tienen entre 20 y 25 años de experiencia, pero siguen trabajando como voluntarias”, dijo Bernis.
El papel de Medi-Cal
Para pagar a los trabajadores de salud comunitarios, Medi-Cal comenzó a cubrir sus servicios en julio de 2022, pero California suspendió un aumento salarial previsto para ellos después que los votantes aprobaran la Proposición 35, que aumentaba los pagos a médicos, hospitales, clínicas comunitarias y otros proveedores.
Desde entonces, el estado aún no ha establecido un sistema uniforme sobre cómo los planes de salud deben contratar a las organizaciones que emplean a trabajadores de salud comunitarios.
“Tenemos que hacer malabares”, dijo María Lemus, directora ejecutiva de Visión y Compromiso, una organización sin fines de lucro con sede en Los Ángeles que representa a estos trabajadores. “Esto sólo causa caos, porque cada plan puede tener requisitos diferentes”.
Lemus agregó que la organización tardó casi seis meses en establecer el pago con un plan de salud.
Y aunque los reembolsos de Medi-Cal están vinculados a tareas individuales, que oscilan entre $9.46 y $27.54 por 30 minutos de trabajo, los activistas afirman que no se les compensa totalmente por el tiempo que dedican a ganarse la confianza de los pacientes y a hacer seguimiento.
Según los activistas, estos trabajadores deberían ganar al menos $30 por visita, con beneficios, pero muchos ganan unos $21 la hora, a menudo sin beneficios.
Lo que sorprende a los activistas es la poca frecuencia con la que se utilizan estos servicios en un programa que cuenta con 15 millones de californianos. Más de 16,000 afiliados a Medi-Cal utilizaron estos servicios durante el primer año, cifra que aumentó a 68,000 el año pasado, según datos del estado. “No creo que se haya alcanzado el potencial del que hablaba el gobernador y que todos imaginábamos que se podría alcanzar”, señaló Sanders.
Griselda Melgoza, vocera del Departamento de Servicios de Salud de California, dijo que la agencia, que administra Medi-Cal, ha observado “una tendencia constante al alza” y cree que los datos subestiman la utilización porque este beneficio a veces se incluye en otros servicios.
Este año se rechazó una propuesta de ley para evaluar si los planes de atención médica gestionada de Medi-Cal realizan la divulgación y educación suficiente entre los afiliados sobre los servicios de salud comunitarios.
Más crucial que nunca
Con los recortes a la financiación de la salud por parte de la administración Trump y la aprobación de la legislación fiscal y de gasto del Partido Republicano, los activistas temen que haya aún menos fondos y apoyo para estos puestos, lo que reduciría las plantillas que se ocupan de las desigualdades en materia de salud.
El Departamento de Salud Pública del condado de Fresno ya ha anunciado el recorte de más de la mitad de sus trabajadores comunitarios: pasarán de 49 puestos a 20.
Sin embargo, la divulgación es más crucial que nunca. Mientras la administración Trump continúa con las redadas de inmigración, que parecen haber tenido como objetivo al menos una clínica en el estado, los activistas y los investigadores advierten que los trabajadores de salud comunitarios podrían actuar como intermediarios para los pacientes inmigrantes que temen buscar atención médica en hospitales y clínicas.
Sin un programa de certificación estatal, sin aumentos salariales y con fondos de capacitación cada vez más escasos, el camino hacia la profesionalización es incierto, lo que hace que esta fuerza laboral se sienta abandonada.
“La comunidad confía en mí”, afirmó Hernández, una veterana trabajadora de salud comunitaria, “pero a nivel gubernamental aún queda mucho camino por recorrer antes de que este trabajo sea valorado y pagado como se merece”.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
from Health Industry Archives - KFF Health News